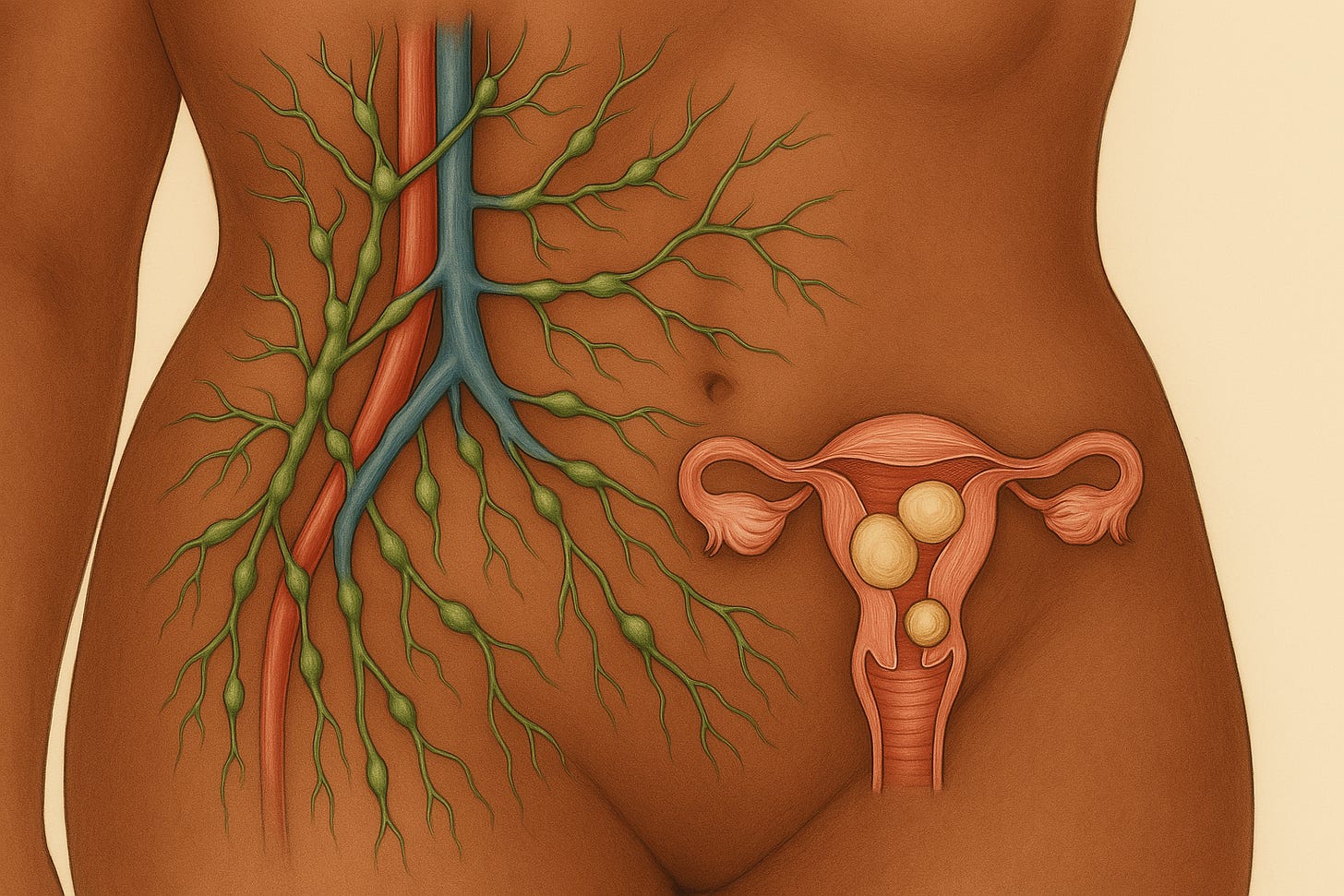
Uterine fibroids are often misunderstood as pathological anomalies, but emerging views suggest they may function more as adaptive responses to chronic physiological stress, particularly involving the lymphatic and digestive systems. Rather than classifying fibroids as a ‘dis-ease’, it may be more accurate to consider them a survival mechanism… a way for the body to buffer against stagnation in waste clearance and impaired cellular turnover.
The Lymph System and Tissue Congestion
The lymphatic system is a crucial but underappreciated aspect of uterine health. Responsible for clearing approximately 30 billion worn-out cells daily, along with metabolic waste and cellular debris, it plays a foundational role in maintaining internal balance. When lymphatic drainage is compromised, mainly due to poor circulation, chronic inflammation, or digestive sluggishness, fluid and waste can accumulate, leading to localised lymph edema.
In the pelvis and abdomen, this stagnation can backflush waste materials into surrounding tissues, including the uterus and ovaries. Over time, this toxic accumulation may encourage the body to encapsulate debris through the formation of fibroid tissue, a form of bio-adaptive storage rather than uncontrolled growth. Essentially, when the lymph system can't evacuate the waste, the body chooses containment through fibroid development.
Your Body Has a Backup Plan
When lymphatic drainage is impaired, the body often resorts to localised swelling or fat deposition as a compensatory mechanism. This can manifest in:
Lymphedema: Chronic lymphatic fluid build-up, often in the limbs, due to damaged or overwhelmed lymph vessels. The tissue becomes swollen, fibrotic, and prone to infection.
Lipedema: A distinct condition involving symmetrical fat accumulation, typically in the legs and hips, often misdiagnosed as obesity. It’s painful and resistant to diet/exercise, and may involve lymphatic dysfunction.
Lipohypertrophy: Fatty bulges or nodules that form in areas of repeated trauma or stagnation; sometimes seen in insulin injection sites or areas of poor circulation.
Localised adipose bulges: These can appear anywhere lymphatic flow is compromised; abdomen, thighs, upper arms, even under the chin. They’re often soft, fibrotic, and may feel heavy or tender.
Think Dr Pimple Popper!
Digestive Dysfunction and Bile Flow
One of the primary contributors to lymphatic congestion is digestive dysfunction, particularly sluggish bowels (constipation) and poor bile secretion. Bile is produced by the liver and stored in the gallbladder, and it acts as a natural cleanser by facilitating the breakdown and excretion of fats and toxins. When bile flow is reduced, often due to bile duct blockages or liver congestion, intestinal transit slows down, leading to constipation and the build-up of internal waste. This, in turn, compounds lymphatic load and impedes efficient drainage from the pelvic organs.
Nutritional Impacts and Blood Vessel Integrity
Dietary choices heavily influence lymphatic and vascular health. High intake of animal protein has been associated with the thickening of blood vessel walls, particularly at the basal membranes where nutrient exchange occurs. When these membranes become rigid or clogged, nutrient delivery to the uterine tissues suffers. Over time, this sets the stage for degeneration and fibrosis.
A plant-forward, low-protein diet may help clear vessel obstructions and improve nutrient absorption in reproductive tissues. Several studies, including those investigating vascular remodelling and fibrosis regression, suggest that minimising dietary protein and inflammatory foods may aid in reversing tissue hypertrophy and restoring vascular elasticity.
The Body’s Innate Capacity to Heal
The body holds a remarkable intelligence, capable of breaking down unnecessary fibroid tissue when metabolic, digestive, and lymphatic circumstances support it. By reducing the lymphatic burden, enhancing bile flow, and optimising circulation, it's possible to create internal conditions conducive to spontaneous regression.
Rather than viewing fibroids as a fixed diagnosis, it's time to reframe them as fluid outcomes; a physical manifestation of internal imbalance that the body can resolve under the right conditions.
If this resonated, here are three powerful articles to explore next:
This space is where I teach the real truths about fibroids, womb health, and healing: the things women are never told. Stay connected as I continue to share the frameworks, insights, and root‑cause teachings that shape my work.
References
Benign metastasizing uterine leiomyoma with lymphatic and pulmonary metastases
BMC Women's Health, 2023Microvascular flow imaging of fibroids: A prospective pilot study
Acta Obstet Gynecol Scand, 2024Impact of serum lipid on recurrence of uterine fibroids
BMC Women's Health, 2024Correlation between inflammatory markers and lipid metabolism in patients with uterine leiomyomas
Frontiers in Medicine, 2023Uterine Fibroids and Diet
International Journal of Environmental Research and Public Health, 2021Diet and Nutrition in Gynaecological Disorders
Nutrients, 2021Uterine Fibroids and Nutrition - Possible Links
Today’s Dietitian