The Quiet Revolution: Why Women are Pushing Back
For decades, the path of uterine fibroid care was paved by an authority-led paradigm that systematically funnelled women toward life-altering major surgeries. Today, we are witnessing a quiet but fierce revolution. A new wave of patient advocacy is reclaiming the narrative, shifting the focus from simply “removing a tumour” to preserving a woman’s identity, health, and future. This movement is a necessary pushback against hysterectomy as the default, which is being driven by women who are no longer willing to accept limited options that prioritise surgical convenience over their long-term quality of life.
This shift is fuelled by five core desires that represent a fundamental reclamation of gynaecological health:
Preserving Your Uterus: Many women view their uterus as vital to their bodily integrity and psychological well-being.
Retaining the organ prevents the profound mental health impact and long-term physiological changes, such as pelvic floor dysfunction or early menopause: associated with sudden removal.
Protecting Fertility: For those in their reproductive years, the diagnosis should not be a death knell for family planning.
Access to fertility-sparing care ensures that medical circumstances do not prematurely dictate the end of a woman’s choice to conceive.
Demanding Less Invasive Care: There is a surging demand for skin-sparing procedures that avoid large abdominal incisions.
Minimally invasive options significantly reduce physical trauma, lowering the risk of life-threatening surgical complications and chronic adhesions.
Accelerating Recovery: In an era where women are economic pillars, six weeks of surgical downtime is often an impossible ask.
Faster recovery returns women to their lives and careers, mitigating the staggering £1.7 billion annual economic impact of sickness absence caused by fibroids.
Autonomy: Women are moving from being passive recipients of advice to being the primary stakeholders in their care.
When a patient is the final authority, she selects treatments aligned with her specific lifestyle, resulting in significantly higher post-treatment satisfaction and a sense of empowerment rather than victimization.
This trend is evidenced by qualitative research showing that women are increasingly turning to the internet and second opinions to fill the gaps left by their primary doctors. However, while the desire for change is strong, systemic barriers and a pervasive information deserts continue to block the path to true informed consent.
The ‘Information Desert’: Why You Haven’t Been Told Your Options
There is a distinct clinical gap between the data patients seek (demand) and the narrow, surgery-heavy resources provided by the medical establishment (supply). Closely linked is Medical Dissonance, a documented clinical ‘paradox’ where 85% of women report appearing comfortable talking to their doctors, yet 84% simultaneously state they do not feel they are being listened to.
The medical establishment frequently funnels women toward major surgery because it is the standard they are trained in, not necessarily because it is the best fit for your life. Strategic barriers prevent many women from pushing back:
Strategic Omission of Alternatives: Non-surgical options like Uterine Fibroid Embolization (UFE) are frequently omitted from first-opinion consultations.
The Hysterectomy Default: Systems are built to favour the most radical options as a permanent fix, ignoring the high long-term personal cost of organ removal.
The Authority Trap: A natural trust in the medical white coat can lead patients to accept limited advice as the only solution.
Crisis-Driven Fear: The physical weight of severe bleeding and pain can make high-level advocacy feel impossible during a crisis.
Diagnostic Exhaustion: In the UK, over half of women experience diagnostic delays of more than two years, and 1 in 4 are offered no treatment at all following diagnosis, according to RCOG data.
Social media often exacerbates this desert. While #fibroids engagement is high, information quality is consistently poor. Research reveals that while open surgical approaches are mentioned in 12.7% of posts, minimally invasive surgery (MIS) appears in fewer than 7%. This lack of representation keeps women in the dark about their right to advanced care. To escape this desert, you must start with a precise clinical map of your own body.
The Knowledge Power-Up: Getting a Proper Assessment
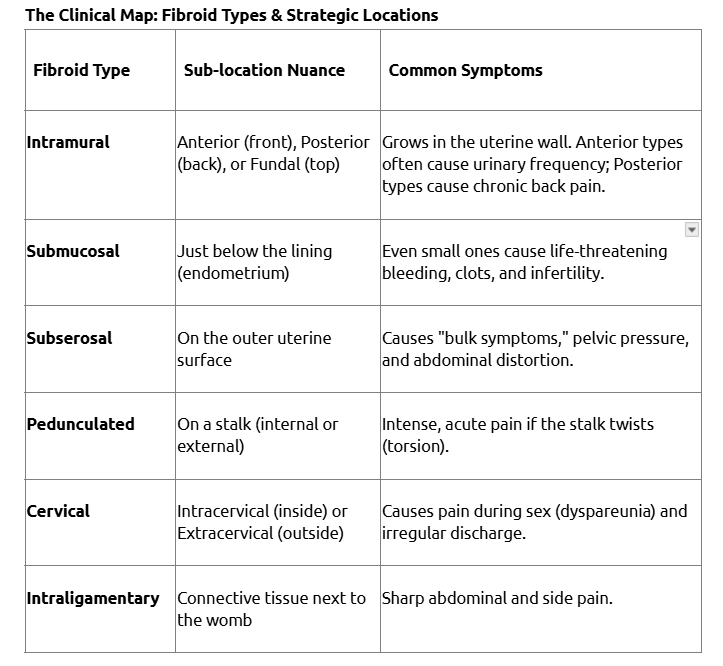
A generic you have fibroids diagnosis is insufficient for modern care. To unlock eligibility for non-surgical treatments, you need a high-resolution clinical map that identifies the exact type, volume, and sub-location of every growth.
Your Assessment Checklist
Do not leave your specialist’s office until the following have been answered:
Exactly how many fibroids are there?
What is the specific volume (size in cm) of the largest ones?
What is the exact map of their locations (e.g., Posterior Intramural vs. Fundal)?
Are any pedunculated or cervical?
Can I have a copy of the raw imaging files or the MRI on a CD? (General reports are often insufficient for a second opinion with a vascular specialist).
The Treatment Spectrum: Navigating Your Alternatives
In modern care, watch and wait should never mean wait and suffer. True care is multi-modal, addressing the environment that allows the fibroids to grow while utilising advanced technology to shrink them.
Holistic & Medical Management
You can actively influence the metabolic drivers of growth through specific cofactors:
The Synergistic Power-Up: Clinical data shows that taking 5,000 IU of Vitamin D alongside 800mg of Green Tea Extract (EGCG) can lead to a significant reduction in fibroid volume and symptom severity.
The Estrobolome Lever: This is the specific subset of your gut bacteria responsible for metabolizing and excreting oestrogen. If your gut is imbalanced, used hormones recirculate and directly fuel fibroid growth.
The Insulin-Fibroid Axis: High insulin acts as a potent growth factor that tells fibroid cells to grow. Managing your metabolic health is fundamental to turning off the growth signal.
Traditional Chinese Medicine (TCM): Formulas like Gui Zhi Fu Ling Tang are clinically proven in trials to reduce volumes and improve cycle balance by addressing the underlying stagnation.
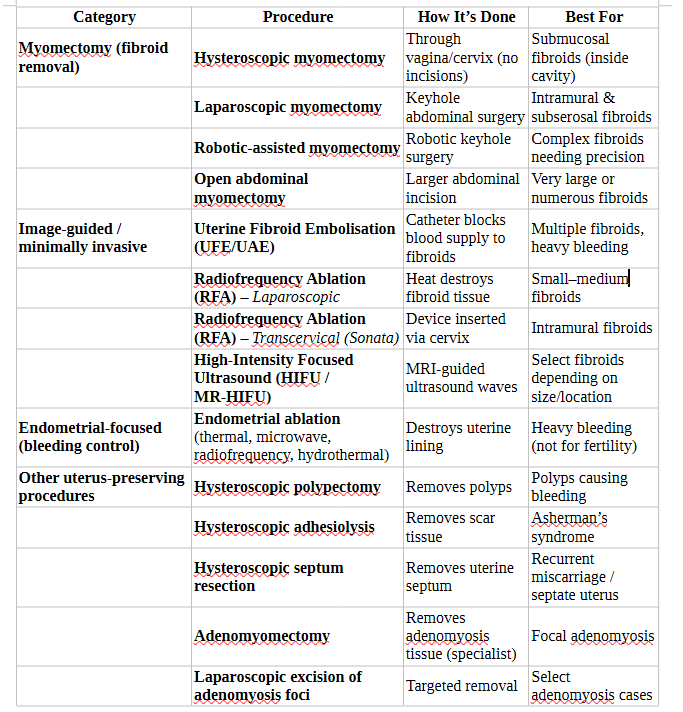
Minimally Invasive & Non-Surgical Options
These are the procedures frequently omitted from the Information Desert.
Surgical Pathways
Myomectomy: (Laparoscopic, Robotic, or Hysteroscopic) The gold standard for fertility preservation. It removes the tumours while keeping the uterus intact.
Hysterectomy: This should only be considered as the very last resort when there are serious complications.
Reclaiming Your Authority: Navigating the Healthcare System
Given that 25.7% of women express active distrust in the medical system regarding fibroids, getting a second, third or forth opinion is your most powerful weapon. If your surgeon only offers a hysterectomy, they are showing you their specialty, and what they are capable of. Nothing more.
The 3-Step Guide to Pushing Back
Demand the Raw Data: Do not settle for a summary. Request your imaging on a CD. Vascular specialists (Interventional Radiologists) often see possibilities in an MRI that a general gynaecologist might miss.
Challenge the Default: Explicitly ask, “Am I a candidate for UFE or RFA? If you don’t perform them, I would like a referral to an Interventional Radiologist or a Vascular Specialist who does.”
Vet the Natural Cures: Distinguish between social media quick fix “cures” and evidence-based programmes such as The Ascension Code.
A Note on Racial Equity: Systemic racism in medicine means Black women face longer delays, more severe symptoms, and are disproportionately represented on surgical waiting lists. If you are a ‘black’ woman, high-intent advocacy is a necessary strategy. You have the right to demand the same range of minimally invasive options and urgent care as anyone else.
Your Path Forward
Modern fibroid care is about preserving your lifestyle, fertility, and bodily autonomy. You are not being difficult by asking for the raw data or demanding a second opinion; you are being an informed partner in a system that is currently failing far too many women.
An informed patient is the medical system’s most valuable partner. By mastering your clinical map and understanding the multi-modal levers of care, you shift the conversation from a generic default to a personalised solution that protects your future.
Your health, uterus, and future are worth the second opinion. Do not wait for your symptoms to dictate your life.
If this resonated, here are three powerful articles to explore next:
This space is where I teach the real truths about fibroids, womb health, and healing: the things women are never told. Stay connected as I continue to share the frameworks, insights, and root‑cause teachings that shape my work.



This is so helpful -- thank you for putting this information out.
I'm wondering if anyone has used Ivermectin, Fenbendazole or Mebendazole to deal with fibroids? They all attack tumor and are having success in cancer cases. I haven't seen anything about this.